![]() In recent years there has been much talk about the need to follow clinical guidelines while developing our medical activities in order to standardize our procedures and act according to the best available scientific knowledge but also to have legal protection for any problem.
In recent years there has been much talk about the need to follow clinical guidelines while developing our medical activities in order to standardize our procedures and act according to the best available scientific knowledge but also to have legal protection for any problem.
In our department, we try to develop new guidelines and put up to date the old ones every year with that goals, as we showed before. This time, the lack of a solid scientific evidence and the fact that different scientific societies give diverse advice hardens the reach of a conclusion.
What seems clear, is that the data obtained in the last years show that progression from Barrett’s esophagus to cancer is actually much lower than we were assuming and that the surveillance intervals could be longer than the ones used untill now. This longer intervals could, paradoxically, prevent more cases of early cancer, as many patients fail to accomplish surveillance due to the high number of endoscopies they have to go through.
We have to think about the importance of the new endoscopic techniques, diagnostic as chromoendoscopy or virtual chromoendoscopy or therapeutic like endoscopic submucosal dissection (ESD) or radio-frequency ablation (RFA) and how their use can modify the application of the guidelines in different places.
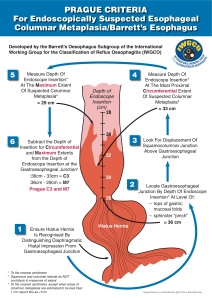
Here i show our recommendations for Barrett’s esophagus screening and surveillance. The complete guideline is inked at the end of the post (in spanish)
NOTE FOR PATIENTS: This guide is developed in a specific department. Your doctor can follow other criteria, which doesn’t mean it’s wrong, so you should discuss with your doctor before following the advice of this guide.
RECOMMENDATIONS
Screening
-We recommend against screening for Barrett’s esophagus (BE) in general population and in patients with gastroesophageal reflux disease (GERD). Patients with GERD with multiple risk factors (age >50y, intraabdominal fat distribution, male…) could be offered screening.
Surveillance
– Endoscopies should be endorsed to a special list endorsed to the Endoscopy Unit and will be done under sedation.
– A white light exhaustive evaluation will be performed preferably with a high-resolution endoscope. If possible acetic acid chromoendoscopy and Narrow Band Imaging will be applied.
Intervals
-BE without dysplasia
-Every 5 years (may be reduced to 3 years if longer than 3 cm. or several risk factors)
-Biopsy of any visible lesion and 4-quadrant biopsy every 2 cm.
– BE with low-grade dysplasia. (Always confirm dysplasia by a second pathologist)
-Every 6 months untill 2 consecutive endoscopies show no dysplasia.
-If there is any suspicion of inflammation, repeat endoscopy after 8 weeks of intensive treatment (twice a day) with proton pump inhibitors (PPI).
-Biopsy of any visible lesion and 4-quadrant biopsy every cm.
-BE with high-grade dysplasia.
-Endoscopic mucosal resection of the visible lesions and RFA of all the BE extension.
-If treatment is not possible, every 3 months, biopsy of any visible lesion and 4-quadrant biopsy every cm.
-Specific cases can undergo esophagectomy in specialized surgical centers.
Treatment
-We recommend PPI treatment at standard dose or the needed dose to maintain the patient asymptomatic.
-Antireflux surgery will be recommended to patients with bad symptomatic control or those who prefer surgery to long-term PPI treatment.
-Acetilsalicilic acid treatment will be individualized to patients with concomitant cardiovascular risk factors after information of risk/benefit.
